“Patient age alone is never a limiting factor.”
We age healthier and live longer than we did a few decades ago. What does this mean for the oral health of elderly patients?
Gerodontology facts
A geriatric patient shows physiological signs of aging, e.g., decline in mobility and function, tactile perception, vision and manual dexterity. These signs are generally progressive and irreversible up to the point that the patient may become dependent on help for their daily activities. When we provide a denture for such a patient, special considerations are necessary. Also, the legal contexts, e.g., patient consent and compliance, are different compared with younger patients.
Gerodontology is a specialty combining all disciplines of dentistry. It also overlaps with other disciplines, e.g., nutrition and public health. We still do not have many independent gerodontology departments worldwide, but the specialty is becoming more recognized, and university structures are adapting.
Our life expectancy has changed over the decades.
Some 50 years ago, geriatric dentistry was barely developed, and there was a reason for that. The average age of the edentulous patient cohort was often 50–60, which is no longer the case.
Now we have studies with 85+ as the patients’ average age. We lose teeth much later in life, due to our healthier lifestyles, and there have been developments in dental materials, implants and regenerative dentistry. If all goes well, we can keep all our teeth right to the end. But due to much longer life expectancy, we may still experience some tooth loss. And edentulous patients are quite different from the ones we had 50 years ago. They are much older! Their mucosa is more fragile and inelastic. Their spongiosa becomes more brittle and affects the alveolar crest. The bony structure of joint articular tubercle is also subject to atrophy, so there are a lot of changes in the temporomandibular joints. We also have loosening of the ligament structures and atrophy of muscle bulk. Patients may lose about 40% of their musculature over their lifetimes, which leads to less precise and less coordinated motor skills. We also see changes in the central nervous system and neuroplasticity, whereby the brain cannot easily adapt to the movement patterns of a new dental arch. All these factors should be considered when we define the occlusion for an elderly persons' prosthesis.
Do teeth age faster than the rest of the body?
The oral cavity is part of the general human organism and may age the same way. Sometimes chronic oral diseases are the first indicators of something happening to the body. For example, with the onset of neurodegenerative disease, we lose weight in a very short time. The first sign is usually when dentures loosen. Patients come to see us, even if denture relining was done just six months previously. Analyses show the patient has weight loss and should be sent for more in-depth evaluations.
Osseointegration happens in older age too.
Elderly patients should benefit from what modern dentistry offers, just like younger patients. Implants are very helpful for elderly patients, e.g., for retention of dentures. We also know that osseointegration happens in older age. In fact, the survival rates for implants are very good – over a 10-year observation period, 9 out of 10 implants will still be in place.¹ Age itself is not a limiting factor for implant therapy. Also, there is no limit to using biomaterials for reducing morbidity.
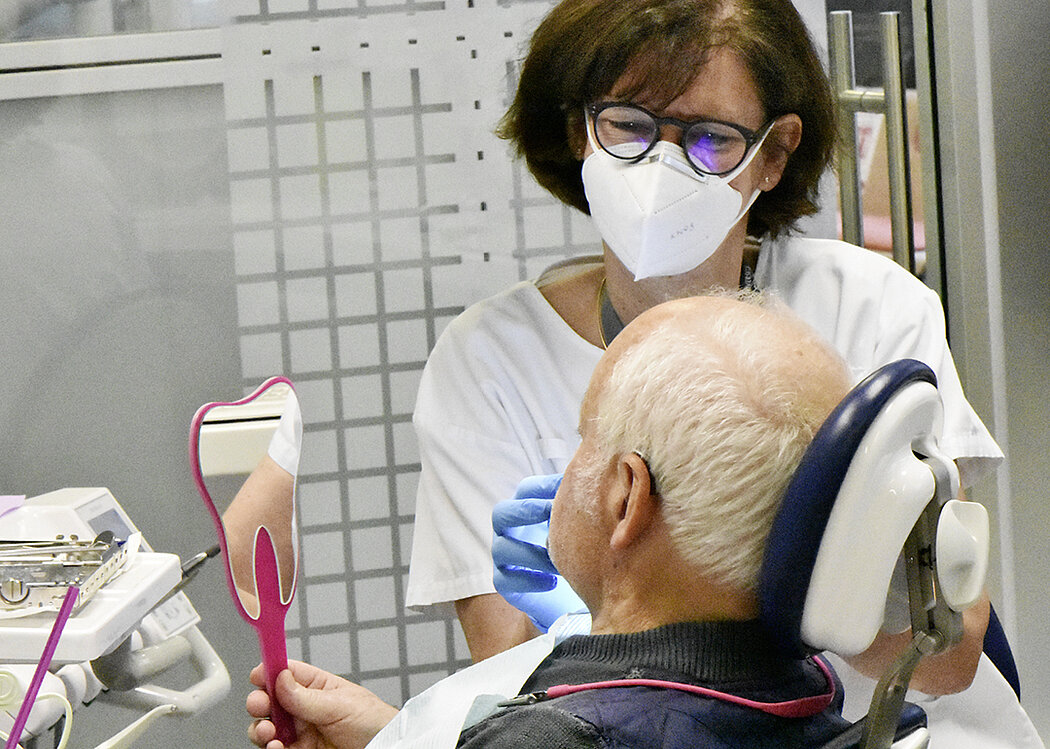
Elderly patients can be less demanding than younger patients, and accept situations that the dentist considers dissatisfactory or requiring urgent treatment.
When an implant is not the first choice.
Sometimes a disease or the side effect of treatments contraindicate implant therapy. Cancer alone is not a contraindication. But when it is treated with radiotherapy or chemotherapy, or when the patient receives antiresorptive, bisphosphonate therapy for the treatment of bone metastases, then implant therapy may not be the best option.
Also, I do not recommend implants when signs of cognitive decline and related deterioration of motor coordination are diagnosed. Alzheimers and dementia are progressive, and we do not have a treatment for them yet. So we need to provide appropriate retention, e.g., with adhesives. It may be less comfortable and less pleasant, but at the end of the day, we will be able to keep the patient’s mouth clean. Without the appropriate oral hygiene, every solid surface in the mouth may crystalize biofilms, which could later cause aspiration pneumonia. In elderly people, oral hygiene has a preventative effect on mortality from pneumonia.²
Complication rate increases with dexterity decline.
We know that the risks of complications in the elderly are similar to those in younger patients as long as the patients can accomplish independent hygiene.¹ The risks increase when they are not able to perform oral hygiene themselves. In this case, we need to accompany our patients along their journey of functional decline, e.g., by de-sophisticating the denture and simplifying retention step-by-step. For example, when the patient is not able to clean the fixed prosthesis anymore, we can change it to a removable prosthesis, probably with bars or stud attachments. When manual dexterity declines further, we can change the abutment for ball attachment, or magnets, and at the end of the process, when the patient becomes too fragile, it may be prudent to remove the abutment, fill the component with provisional reline, and prescribe denture adhesives.
Compliance and the paradox of geriatric dentistry.
Elderly patients are a dentist’s dream customers. They are punctual, they have time for follow-up visits, and they still believe in the white coat, which means they take doctors’ advice very seriously. And they can also be less demanding than younger patients. We call this the “paradox of geriatric dentistry”, whereby patients better accept situations that the dentist considers dissatisfactory or requiring urgent treatment. This attitude may create a discrepancy between treatment need and demand. Nevertheless, the patient’s inability to follow our instructions, due to their dexterity, functional or cognitive decline, should not be considered “non-compliance”. Above 90, one out of three patients may have dementia. Although we may see the first signs, diagnosis should be confirmed by a specialist. Yet diagnosis is important, because it will have a big impact on our treatment planning. Approximately 6–8 years may pass between diagnoses of dementia and death, and towards the end the patient may not be able to comply with hygiene measures or dental treatments. This is why dementia patients have more untreated caries and/or periodontal disease, a higher prevalence of tooth loss and also difficulties using their dentures.
We can’t leave these patients alone.
Professional ethics oblige us to follow the patients and make sure they have access to care and oral hygiene. As these patients generally visit their doctors more often than their dentist, physicians and also family members can help detect issues. We need manpower for primary screening, and it is easy to train a family member to supervise the patient or support them when dependency increases. Most patients arrive at our office accompanied by a son, sister or partner who is somewhat fitter. We train these “caregivers” how to supervise oral hygiene or handle dentures, and we point out the weak points and important issues, along with what they need to do when they occur.
Digital dentistry is the future.
Of all technical advances, digital dentistry has made the biggest impact on gerodontology by bringing access to many more patients in rural areas and institutions. Clinical situations can be documented and sent to the diagnostic or support center. The workflows are much faster and reduce waiting time. With intraoral scanners, chair-time is much easier for patients who are afraid of impression- taking, gagging, and vomiting. And ultimately, we can provide the patient with a cost-efficient denture that is very similar to high-end prosthetics. 3-D printed dentures are versatile, accessible and comparable to milled, completely removable prostheses.³ In a double-blind, randomized, crossover study, we asked patients which dentures they preferred to keep, 3-D printed or milled, with both options available free of charge. The milled denture needed more adjustment in terms of clinical chairside time. Also, professionals could see the differences and say the printed denture was not as pretty. But it was quite amazing how patients liked both dentures similarly.
We can save the printed denture file on a computer and reprint it again when the denture is lost in the nursing home – something that happens quite often. Also, the price is attractive. Based on data from Switzerland, the printing cost is one-third of what a dental technician would charge, so the patient saves money by using CAD/CAM techniques. And in the near future when the price falls further, traditional relining technology will be more expensive than milling a new denture.
Esthetics are important at any age.
We did a hypothetical study, where we asked a young and an elderly cohort: “If you had a denture, would you like it to look like the teeth you have now, or would you take the opportunity to have bright white flawless teeth?”⁴ The results were amazingly similar. Two-thirds of each group wanted to have a natural appearance consistent with their age, and one-third said they would choose white teeth aligned like a string of pearls. And esthetics is where patients should always have the last word!
Elderly patients are full of stories.
Every moment with elderly patients is special and unforgettable. I remember one of my patients with an implantsupported denture that he could not insert easily since his stroke. After adjustments I placed the denture easily. He looked at me and said, “Wow, if you keep up this good work, one day you are going to be somebody!"
References